- Home
- |
- About Us
- |
- News and Events
- |
- Resources
- |
- Contact
- |
- Donate today
Areas of interest

Amputation is life changing and can be a catastrophic change to your function and mobility. Contacting Limbs 4 Life and their team of Peer Support workers is always a step in the right direction, especially for information regarding what the future holds and how soon things will start to turn around. But you may feel that your own journey is private and the next twelve months will be yours to own. A Prosthetist sees amputees on their journey from immediately post-operative, right through to achieving goals both big and small. No journey is identical and none more important than your own.
The cause of your amputation can sometimes mean healing times and potential issues are predictable, but there are variables. It is very rare that an amputation is completed without there being co-morbidities (the presence of one or more diseases) that can affect healing. Generally, a vascular amputation will heal much slower than a traumatic amputation for an otherwise healthy individual, however associated injuries can also slow the rehabilitation process. Over the past 25 years I have seen traumatic amputations heal with primary intention (see the meaning below) in 7-10 days and have also seen vascular clients all healed up at 21 days, but generally I would expect average times from surgery to sutures out, to be 3-4 weeks. Primary intention means the wound heals together entirely with the first closure. But it is more common in vascular clients to have small slower areas of secondary intention healing to wait for. If your wound is slower to heal add a couple of weeks for the wound to strengthen.

Volume Management
When the sutures are removed it’s time for your rehab team to discuss further management of the oedema (swelling) and also improving the shape of your stump for your first prosthesis. A trans-tibial or below knee amputee may have already been fitted with a Rigid Removable Dressing (RRD), a common practise to begin management of stump volume, whilst also protecting the healing suture line. If an RRD has been used, then a compression garment called a “Shrinker” can generally be applied straight away and the RRD worn straight over the top. Sometimes the shape of the limb determines whether a Shrinker is optimal, or stump compression bandaging is the way to go. Either way, once the sutures are out and the Rehab team are talking about a prosthesis, you will then need to manage the volume of your stump in preparation for successful rehabilitation.
Prosthetists who manufacture the first prostheses (Interim prosthesis) prefer you to have mastered Donning (putting on) and Doffing (taking off) the Shrinker and to have been wearing it without issue for 1-2 weeks minimum. It’s not uncommon for you to be at home during the healing process and it will be up to you to make sure the stump is protected, and any volume management process is strictly adhered to. An appointment can then be made with a Prosthetist to assess and then cast your stump to create your first prosthesis.
You can expect a cast for your first (Interim) prosthesis to occur between 1-4 weeks post suture removal and only when the stump is given clearance for loading. The better the healing process up to this point, the quicker you will master the prosthesis. This includes all types of amputations of the upper and lower limbs. A cast is used to create your first limb based on the design inputs you supply, these include your amputation type, the length of the stump, tissue type, your general health and strength, your physical health, skills, dexterity, body weight, your goals and the environments where you will be using the prosthesis. Most centres will try to minimise the time between casting and fitting, and this may range from 1 to 14 days. Expect one week average, unless you have very particular custom needs of the component parts, such as a “special order” foot, or you are trialling a multi-articulating hand.
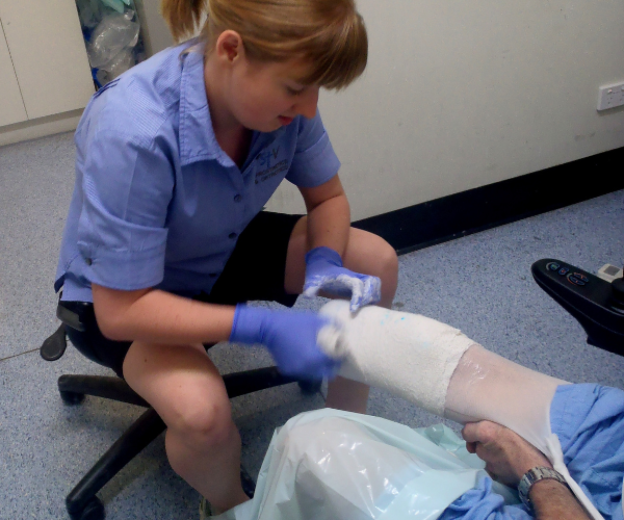
Once you have been fitted with a lower limb prosthesis your stump will really start to change. The action of weightbearing through the tissues of your stump pumps the swelling (oedema) from your tissues and expedites the healing process… but be careful not to overdo it! You must always stop while it still feels okay. Experienced therapists are essential at this stage, as is the importance of sticking to a routine and being vigilant with skin checks. Your Physiotherapist will provide you with a wearing regime if you are a leg amputee, while an experienced Occupational Therapist will generally be the person to assist with upper limb training.
Managing the volume of the stump is essential to keeping the prosthesis fitting well and protecting your stump. Adding socks is the best way to counter the loss of volume whilst walking, and can be done wherever you are, no excuses! If sock changes don’t make improvements, it’s time for your Prosthetist to change the shape of the socket through simple packing or sometimes a new socket is required. The Interim process generally continues until you have stabilised and found a routine in your activities. The process is different for all amputees, as are the processes available throughout Australia. I generally don’t expect any lower limb amputation to stabilise within the first 6 months.

Generally, you will need 2 interim sockets in the first 6-12 months for lower limb prosthetics. If you have lost an arm your first socket may fit for a bit longer, depending on how much swelling was present when it was cast. A person with an upper limb amputation will also usually find that their stump matures well when using the prosthesis daily. This stump maturation through prosthetic use is ideal and can contribute to better control and a more successful outcome.
So, it’s 6 months after your amputation and you may be wearing a prosthesis every day, all day, or just to complete simple tasks for a few minutes. Either way, a prosthesis is now part of your life, as is your Prosthetist, who will generally be the one health professional you will form a long connection with. This relationship is important and comes with all the privacy and professionalism you should expect from any healthcare provider. Make sure you are happy with your Prosthetist, otherwise find someone else. It’s too much of an important relationship for you not to own the decision. Some of you may only be up on a prosthesis for the first time, 12 months after your amputation or still waiting! The timing doesn’t matter. If you are engaged in your care, have insight into your specific challenges and can stick to a rehab plan, you will improve. If you are caring for someone with limb loss and they seem to be moving very slowly through the processes, don’t be afraid to ask treating team members what the goals are and how can you help. Clearly communicated goals help everyone.

When everything goes right you will be fitter and healthier than you’ve been in a long time. You may be mobile on a prosthesis, back into life with a wheelchair, using a new arm to hold the kids or just enjoying life away from a hospital. Either way, your world can start to assume a new normal.
Keep up to date with our latest news, events and information